Waking up tired after what should have been a full night of sleep can wear you down in ways people around you don't always see. You may be relying on coffee, feeling foggy in afternoon meetings, or hearing from a partner that your snoring and pauses in breathing are getting worse. For many adults in Walnut Creek and the East Bay, that cycle leads to the same question: what are the best sleep apnea solutions if CPAP feels overwhelming or has not worked?
That's where dental sleep medicine can make a meaningful difference. A well-chosen treatment should do more than look effective on paper. It has to be something you can comfortably use night after night. For many people with mild to moderate obstructive sleep apnea, and for many people who are CPAP-intolerant, a custom oral appliance is often the most practical path back to steady, restorative sleep.
Finding Restful Sleep Again in Walnut Creek
A common story sounds like this. You go to bed on time, sleep for hours, and still wake up feeling like you barely rested. By midmorning, you're dragging. By evening, you're frustrated. If a spouse or partner has noticed loud snoring, restless sleep, or breathing pauses, it can add worry to an already exhausting problem.

In my experience, people usually don't come in asking for a technical explanation first. They want relief. They want to know if there's a solution that won't make sleep harder than it already is. They want to know whether they can stop dreading bedtime, stop disturbing their partner, and start feeling like themselves again.
That concern is reasonable. Sleep apnea treatment should be effective, but it also has to fit real life. If a device is too noisy, too bulky, or too difficult to tolerate, even a strong treatment can fail in practice because it ends up sitting unused.
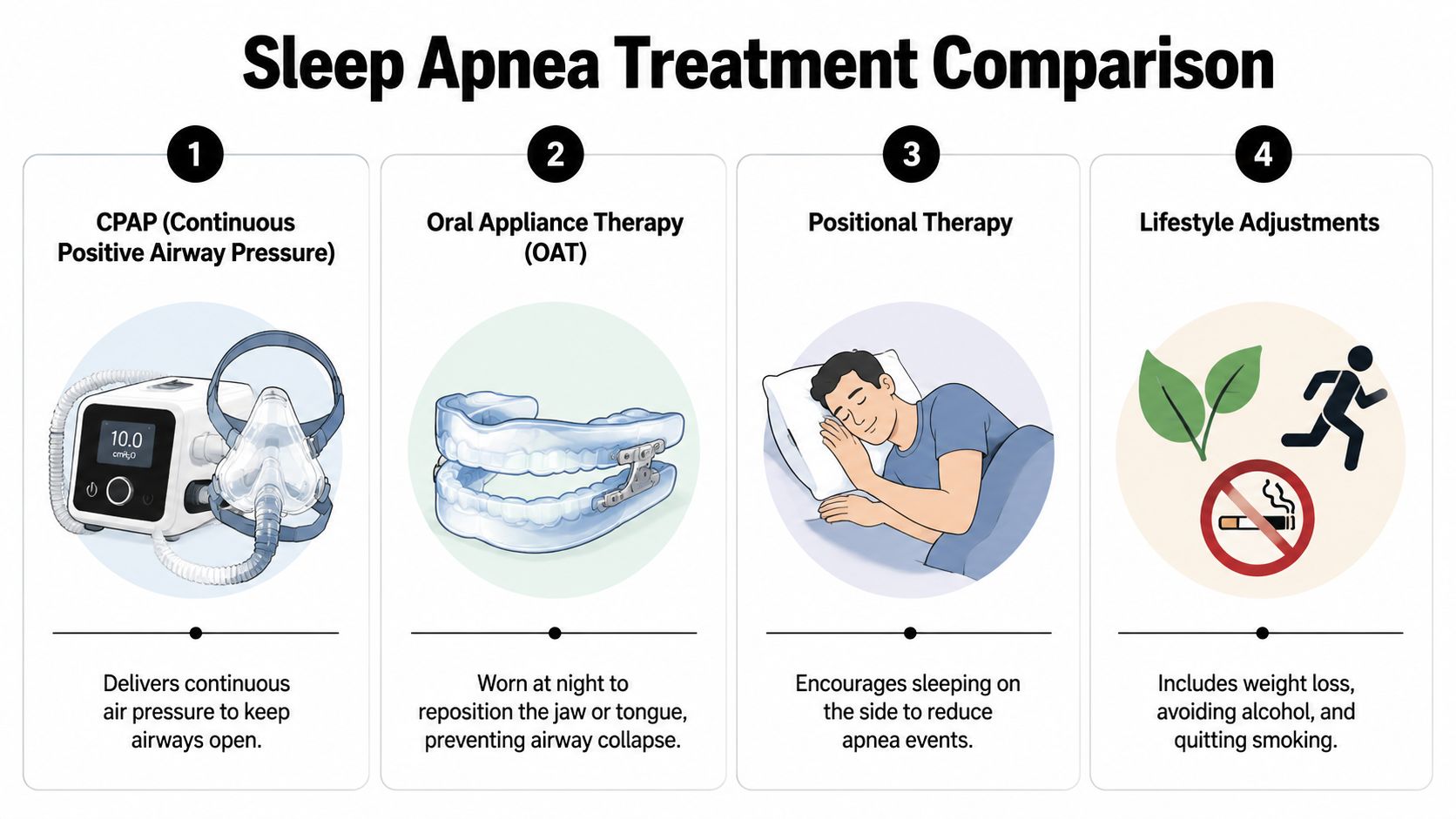
A quick comparison of the main options
| Treatment | How it works | Often a good fit for | Main trade-off |
|---|---|---|---|
| CPAP | Uses air pressure to keep the airway open | Moderate to severe cases, especially when patients tolerate it well | Very effective, but many people struggle with long-term use |
| Oral appliance therapy | Repositions the jaw to help prevent airway collapse | Mild to moderate cases and many CPAP-intolerant patients | Requires custom fitting and follow-up adjustments |
| Positional therapy | Reduces airway blockage linked to sleeping position | People whose apnea is worse on their back | Helpful for the right pattern, but not enough for everyone |
| Lifestyle changes | Supports overall airway health and sleep quality | Patients who need a broader long-term plan | Useful support, but usually not a stand-alone fix |
| Surgery or implanted therapy | Changes anatomy or airway muscle behavior | Selected cases after careful medical evaluation | More invasive and not the first choice for many patients |
Better sleep usually comes from the treatment you can actually live with, not just the one that sounds strongest in theory.
Walnut Creek patients often want a solution that feels manageable from the first night forward. That's why comfort, simplicity, and consistency matter so much.
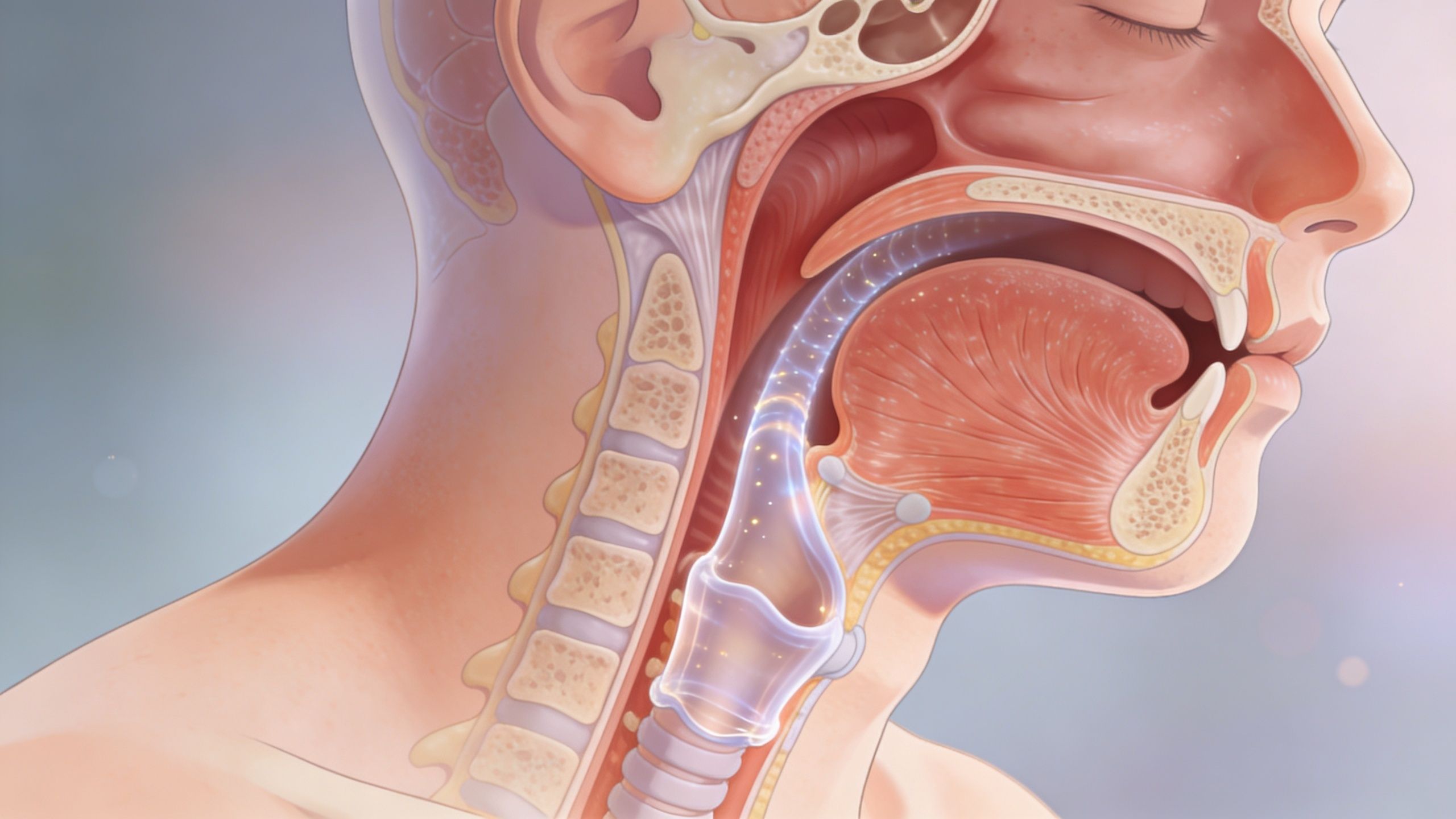
Understanding Sleep Apnea and Its Diagnosis
Obstructive sleep apnea, or OSA, happens when the airway narrows or closes during sleep. The simplest way to think about it is this: the throat soft tissues relax, the breathing passage gets blocked, and airflow stops or drops until the brain briefly wakes the body enough to breathe again. Those interruptions can repeat over and over through the night, even if you don't remember them in the morning.
What it can feel like
Some people come in because of snoring. Others come in because they feel exhausted, wake with a dry mouth, or have trouble staying alert during the day. A partner may notice gasping, choking sounds, or long pauses in breathing before the patient realizes anything is wrong.
If that sounds familiar, it helps to learn the difference between occasional snoring and something more significant. This overview of chronic snoring and sleep apnea warning signs gives a useful starting point for understanding when it's time to be evaluated.
Why diagnosis matters
The most important first step is getting the diagnosis right. Consumer sleep trackers can be interesting, but they aren't enough to guide treatment. According to a review in the National Library of Medicine, consumer devices show high sensitivity of at least 0.93 for detecting sleep opportunity, but their specificity is low, which means they often mistake wakefulness for sleep. The same review notes that polysomnography, or PSG, remains the gold standard before fitting a dental appliance for sleep apnea, as detailed in this analysis of consumer sleep-tracking performance compared with PSG.
If you suspect sleep apnea, the right question isn't “Which gadget should I buy?” It's “How do I get an accurate diagnosis?”
What a sleep study usually involves
A sleep study measures breathing patterns, oxygen changes, and sleep disruption. Depending on your case, the testing may happen in a sleep lab or with an approved home sleep test arranged through your physician. The goal is to confirm whether apnea is present and how severe it is.
That information shapes treatment decisions. It helps determine whether CPAP should be the first recommendation, whether a custom oral appliance may be appropriate, and whether other factors such as sleep position are playing a meaningful role.
For many patients, the testing itself is less intimidating than they expected. The bigger relief comes after diagnosis, because once the problem is clearly defined, treatment stops feeling like guesswork.
A Detailed Comparison of Sleep Apnea Treatments
A patient may come in exhausted, frustrated, and ready to give up after trying a CPAP mask for a few nights. That does not mean treatment failed. It means the first option may not match the way that patient sleeps and lives.
The useful comparison is not which treatment sounds strongest on paper. It is which one improves breathing and fits into real life well enough to be used night after night.
CPAP for the highest pressure-based control
CPAP keeps the airway open with pressurized air delivered through a mask. For many moderate to severe cases, it remains the standard starting point because it can control breathing events very effectively when it is worn consistently. According to data compiled by Floto Group on CPAP device effectiveness and AHI benchmarks, CPAP can produce up to a 95% reduction in AHI.
That level of control matters. I still consider CPAP an excellent tool for the right patient.
The trade-off is tolerance. Some patients do well with the mask, pressure, tubing, and cleaning routine. Others struggle with dryness, leaks, claustrophobic feelings, skin irritation, noise, or the simple burden of setting up a machine every night. A treatment can be clinically strong and still be hard to live with.
Oral appliance therapy for patients who need a treatment they will actually wear
A custom mandibular advancement device fits over the teeth and holds the lower jaw in a position that helps keep the airway more open during sleep. For mild to moderate obstructive sleep apnea, and for many patients who cannot tolerate CPAP, this is often the better long-term answer because comfort and adherence are so much better.
This option deserves more respect than it sometimes gets. It is not just a backup for people who failed CPAP. In the right case, it is a practical first-choice treatment that balances effectiveness with nightly use.
Oral appliance therapy is often a strong fit for:
- Mild to moderate OSA
- Patients who cannot sleep with a CPAP mask
- Frequent travelers
- People who want a quiet, simple bedtime routine
- Patients looking for a less invasive solution they can maintain long term
Its limitations should be stated clearly. It is not ideal for every airway pattern or every severity level, and it needs proper fitting, gradual adjustment, and follow-up to work well. A custom device provided through a dentist who focuses on dental sleep apnea treatment options is very different from an over-the-counter mouthpiece.
Positional therapy for patients whose apnea worsens on their back
Some patients have breathing problems that become much worse in one sleep position, especially supine sleep. In those cases, positional therapy can help by reducing time spent on the back and lowering the number of airway collapse events.
This can be helpful, but it is usually not the whole answer. If obstruction happens in multiple positions, positional therapy alone often falls short.
Practical rule: If sleep position is a major driver of your apnea, position changes may help. If your airway closes in several positions, you usually need a treatment that gives more consistent support.
Lifestyle measures that help but rarely replace treatment
Weight loss, limiting evening alcohol, and improving sleep habits can all support better results. Those changes may reduce strain on the airway and improve sleep quality overall.
Patients deserve an honest explanation here. Lifestyle measures are helpful, but they often do not solve established obstructive sleep apnea by themselves. They work best alongside a direct treatment such as CPAP or a custom oral appliance.
Surgery and implanted therapies for selected cases
Surgery and implantable options have a real place in care, especially when anatomy is a major factor or other treatments have not worked. They can be effective for carefully selected patients.
They also involve more commitment. Recovery time, cost, and variable results make these options less appealing as a starting point for many people, especially when a non-surgical treatment may control the problem well.
How to judge the best option
The best treatment is the one that matches both the diagnosis and the patient. Severe OSA with good CPAP tolerance often points toward CPAP. Mild to moderate OSA, or repeated CPAP intolerance, often points toward oral appliance therapy because a comfortable treatment that gets used consistently usually helps more than a stronger treatment left on the nightstand.
That is the difference patients in Walnut Creek often care about most. They want treatment that works in real life, not only in theory.
How Your Walnut Creek Dentist Provides a CPAP Alternative
For patients who are tired of hearing that CPAP is the only serious option, the conversation changes now. A custom oral appliance isn't a generic mouthguard. It's a carefully designed medical device that helps hold the lower jaw in a position that supports a more open airway during sleep.
Why this works for many CPAP-intolerant patients
The biggest difference is usability. According to this review of current sleep apnea treatments and CPAP alternatives, nearly 50% of CPAP users quit, while oral appliances show long-term adherence rates of 80% to 90% and can reduce AHI by over 50% for many CPAP-intolerant patients.
That matters more than people sometimes realize. A treatment with strong clinical performance but poor nightly use can lose ground to a treatment with slightly lower ideal performance but much better real-world consistency.
At William M. Schneider, DDS and dental sleep apnea treatment options, the role of the dentist is to make that alternative precise and comfortable. The appliance is custom fitted, adjusted over time, and coordinated with your diagnosis rather than handed out as a one-size-fits-all solution.
What the appliance actually feels like
Most patients describe oral appliance therapy as much less intrusive than they expected. There's no mask, no hose, and no machine at the bedside. The appliance is small, quiet, and easy to bring into a normal bedtime routine.
That doesn't mean there's no adjustment period. Some people notice temporary jaw tightness, mild bite changes in the morning, or tooth pressure while adapting. Those issues are exactly why follow-up matters. The goal isn't just getting an appliance made. The goal is fine-tuning it so you can use it comfortably and effectively.
Here's a closer look at how dental sleep treatment is commonly explained to patients:
When a dental solution may be the better first choice
For many busy adults in Walnut Creek, convenience isn't a minor detail. It determines whether treatment lasts. If your schedule is packed, you travel often, or you already know you won't sleep well attached to a machine, oral appliance therapy may be the more realistic starting point for mild to moderate OSA.
The right treatment should lower your symptoms without turning every night into a struggle.
This is especially true for patients who have already tried CPAP and stopped using it. In those cases, a custom oral appliance is often not a fallback. It's the first treatment they're willing to use consistently.
The Lifestyle Benefits of a Dental Sleep Solution
A good sleep apnea treatment has to work in real life, not just on paper. Patients usually notice the day-to-day benefits before they think about anything technical. Bedtime feels calmer. A spouse is no longer listening to machine noise. Packing for a weekend trip takes seconds instead of planning around equipment.
For the right patient, that ease matters because it supports long-term use. I see this often with adults who could not tolerate CPAP but do very well with a custom oral appliance. In mild to moderate cases, the best treatment is often the one you can wear comfortably and consistently for years.
Daily life tends to improve in practical ways:
- Less disruption at night: No bedside machine, no tubing, and no mask shifting if you change positions.
- Better for travel: The appliance fits easily into a small case, which makes business trips, vacations, and overnight visits much simpler.
- Easier bedtime routine: Cleaning is straightforward, and there is less setup before sleep.
- More natural for many patients: A custom-fitted appliance often feels less intrusive than pressurized airflow and face gear.
These details may sound small. They are not.
Treatment only helps if it becomes part of your routine. A dental sleep solution removes many of the obstacles that cause people to give up. Patients are often relieved that they can read in bed, talk briefly with a partner, turn to their side, and settle into sleep without feeling tethered to a device.
There are trade-offs, and patients deserve an honest explanation. Some people need a short adjustment period. Some notice temporary jaw stiffness or morning bite changes, especially early on. Those issues are usually manageable with proper fit, careful adjustments, and follow-up. For a patient who has already decided CPAP is not realistic, those trade-offs are often far easier to live with than a treatment they avoid altogether.
That is why oral appliance therapy is more than a backup option in many Walnut Creek cases. It gives CPAP-intolerant patients a comfortable, effective path they are much more likely to stay with, and that steady use is what leads to better sleep, better energy, and a quieter, less stressful night at home.
Your Sleep Apnea Journey at Our Walnut Creek Practice
Starting treatment feels easier when you know what the process looks like. Most patients want a clear plan, not surprises. The path to a custom dental sleep solution is usually straightforward and personalized.
Step one is the consultation
The first visit focuses on symptoms, sleep history, medical diagnosis, and whether a dental appliance is an appropriate option. We also look at your teeth, gums, jaw joints, and bite because a sleep appliance has to work with your oral health, not against it.
If you already have a diagnosis and are struggling with CPAP, that helps guide the discussion. If you're early in the process, diagnosis through your physician or sleep specialist comes first.
Step two is digital planning and custom fabrication
If you're a good candidate, records are taken so the appliance can be made specifically for your mouth. Patients often appreciate that this process is designed around comfort and accuracy.
The device is then fabricated to fit securely and comfortably. Once it's ready, you return for fitting and instructions on how to wear it, clean it, and ease into treatment.
Step three is adjustment and follow-up
This part matters. Oral appliances often need small refinements so the jaw position balances comfort and airway support. Follow-up visits help address soreness, bite changes, or fit issues before they become frustrating.
In selected mild cases, modern non-invasive options may also be part of the conversation. As noted in Henry Ford Health's discussion of CPAP alternatives including daytime tongue stimulation, daytime tongue stimulation can be integrated with oral appliances as part of a broader approach to managing mild OSA.
Good sleep apnea care doesn't end when the appliance is delivered. It improves through adjustments, communication, and follow-through.
What the experience feels like
Patients in Walnut Creek often tell us they appreciate clear explanations and a calm pace. That matters, especially if you're already tired, discouraged, or anxious about treatment. The goal is to make each step understandable, gentle, and worth your effort.
If you're also looking for a long-term dental home, it's helpful to know that sleep apnea care can sit alongside a full range of dental services such as cleaning and exams, restorative dentistry, cosmetic dentistry, and ongoing oral health monitoring in one familiar office.
Frequently Asked Questions About Sleep Apnea Solutions
Is an oral appliance for sleep apnea covered by medical insurance
Coverage varies by plan. Because sleep apnea is a medical condition, oral appliance therapy is often handled differently from routine dental benefits. The key point is that coverage usually depends on diagnosis, documentation, and plan rules. Before starting, it's smart to verify benefits, required records, and any preauthorization steps.
What are the potential side effects of an oral appliance
Most side effects are manageable and tend to be mild, especially when the appliance is properly fitted and adjusted. Patients may notice temporary jaw soreness, tooth pressure, extra saliva, dry mouth, or a bite that feels different in the morning. These issues should be discussed early so the appliance can be adjusted rather than abandoned.
How long does a custom dental appliance for sleep apnea last
There isn't one fixed lifespan for every appliance because durability depends on the material, your bite, grinding habits, fit, and how well the device is maintained. Some last longer than others. The practical approach is regular follow-up so wear, retention, and comfort can be checked before the appliance loses effectiveness.
If you've been searching for a dentist near me or a dentist in Walnut Creek, CA who can help with sleep apnea as part of dental care, the next step is a conversation about your diagnosis, your symptoms, and what treatment you can realistically use long term.
If poor sleep, snoring, or CPAP frustration is affecting your life, schedule a consultation with William M. Schneider, DDS. Our Walnut Creek practice provides patient-focused dental care with thoughtful sleep apnea solutions, along with a full range of services including cleaning and exams, restorative dentistry, cosmetic dentistry, dental implants, and support for patients who want a comfortable, long-term dental home in the East Bay.