A whiter smile often starts with a simple thought. You have a wedding coming up, an important presentation, family photos, or you are just tired of seeing coffee and tea stains in the mirror. Then the hesitation sets in. You want brighter teeth, but you do not want that sharp little “zing” that can follow whitening.
That concern is reasonable. Many people searching for a cosmetic dentist near me or a dentist in Walnut Creek, CA are not worried about whitening results alone. They are worried about comfort, too. For new patients, sensitivity is often the question they ask first.
The good news is that there are reliable ways to make whitening more comfortable. Some steps start before treatment. Others help in the first day or two afterward. A few matter most if your teeth have always been a little reactive to cold drinks, sweet foods, or air.
If you are weighing store-bought strips against professional care, a practical starting point is this real guide to teeth whitening. It helps frame the trade-offs between convenience, speed, and comfort.
Knowing how to reduce tooth sensitivity after whitening is not about one trick. It is about making good choices across the whole process, from preparation to recovery to follow-up if something does not feel right.
A Brighter Smile Without the Discomfort in Walnut Creek
In Walnut Creek, many adults want whitening for the same reason they want clean, natural-looking dental care. They want to look refreshed without making their routine harder. A brighter smile can help you feel polished at work, comfortable in social settings, and more confident in photos.
What stops people is usually not the idea of whitening itself. It is the fear that sensitive teeth will make the experience miserable for a few days afterward. That fear grows if you have ever felt discomfort from ice water, cold air, or even brushing near the gumline.
The concern behind the question
Sensitivity after whitening can feel surprisingly personal. One patient describes it as a cold flash. Another says it feels like a quick electric spark. Someone else notices only mild tenderness when sipping coffee.
Those different reactions matter because whitening is not one-size-fits-all. Teeth with thin enamel, exposed dentin, old restorations, or baseline sensitivity often need a more careful plan.
Key takeaway: Whitening does not have to be an all-or-nothing decision. Comfort improves when treatment is matched to the patient, not when the patient is forced to adapt to a generic kit.
What comfortable whitening usually looks like
A comfortable whitening journey usually includes:
- Pre-treatment preparation: Sensitive teeth respond better when you start with the right toothpaste and realistic timing.
- A sensible recovery period: The first day or two after whitening matters. Food, temperature, and brushing habits can either calm things down or keep irritation going.
- A plan if sensitivity lasts longer than expected: Most cases settle quickly, but persistent pain should not be ignored.
People looking for a dentist near me often focus on convenience. For whitening, comfort should be part of that search. The right approach protects your enamel, keeps the gums calm, and helps you get cosmetic results without turning the next few days into a struggle.
Understanding Why Your Teeth Feel Sensitive After Whitening
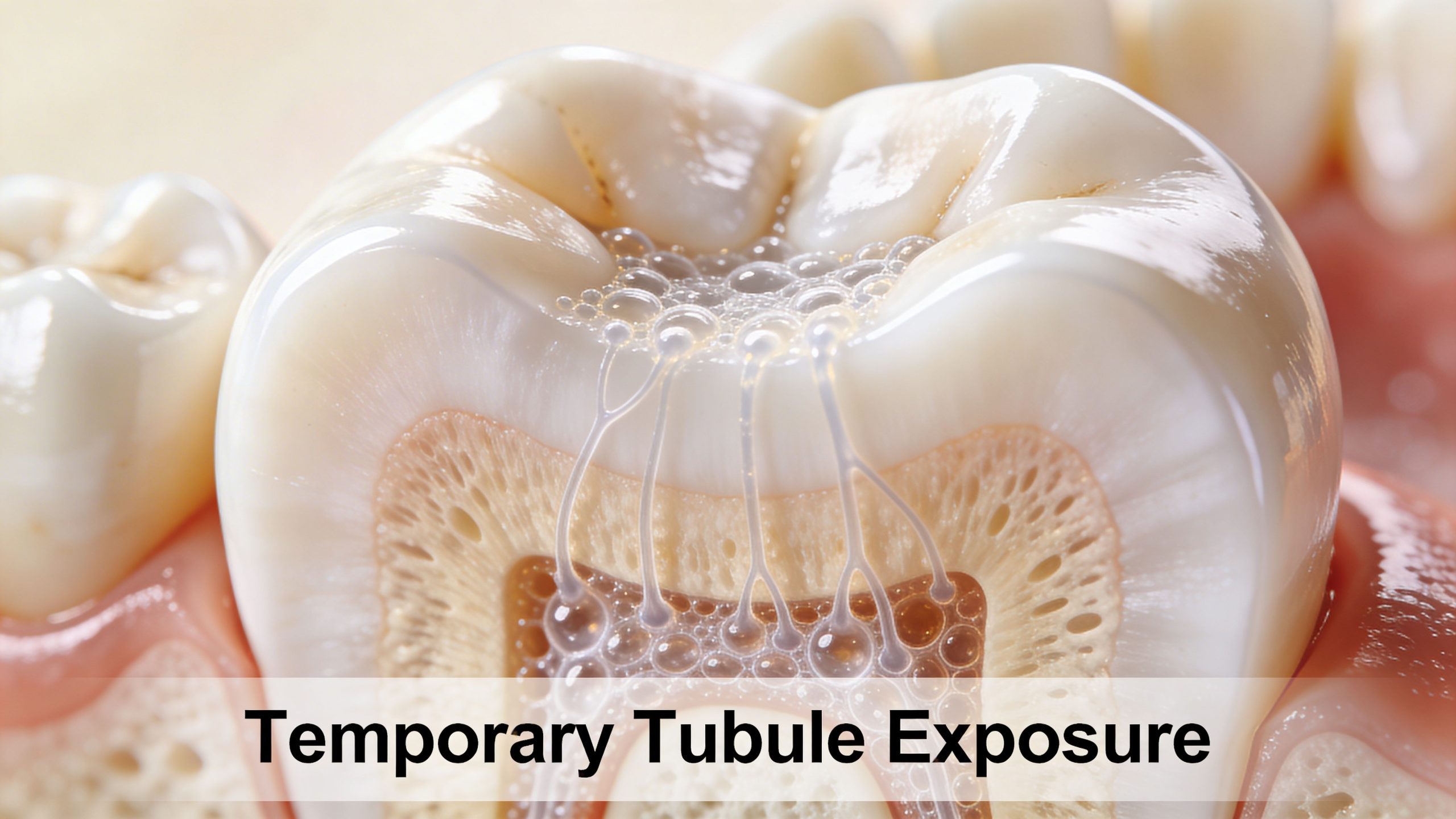
Whitening works by allowing peroxide-based gel to move into the tooth and break apart stain molecules. That same process can temporarily make the tooth more reactive. The easiest way to picture it is to think of whitening as opening tiny pathways in the tooth for a short time.
Those pathways are called dentin tubules. When they are more exposed, hot, cold, sweet, or air can reach the nerve more easily. That is why you may feel a quick sting after whitening even if your teeth looked and felt normal before.
What is normal and what is not
Sensitivity after whitening is common, but that does not mean every level of discomfort is the same. A clinical study found that up to 78% of patients report some sensitivity after whitening, but it is usually mild and temporary. In that same study, about 10% experienced moderate sensitivity and only 4% reported severe sensitivity lasting for a couple of weeks (PubMed).
That tells patients two useful things. First, feeling some sensitivity does not mean something has gone wrong. Second, severe or lingering discomfort is much less common and deserves attention if it happens.
Why some teeth react more than others
A few factors tend to make whitening feel stronger:
- Existing sensitivity: If cold water already bothers you, whitening can amplify that response.
- Higher-concentration products: Stronger gels can produce faster changes, but often with a comfort trade-off.
- Gum recession or exposed root surfaces: These areas are naturally more reactive.
- Aggressive brushing or abrasive products: They can leave the tooth surface more vulnerable before you even start whitening.
If cold drinks have bothered you before, this overview of what causes tooth sensitivity to cold can help connect the dots between everyday sensitivity and whitening sensitivity.
The reassuring part
Whitening sensitivity is usually a temporary biological response, not permanent damage. Teeth often feel “thirsty” after bleaching. As they rehydrate and settle, those sensations typically fade.
Practical point: The more you understand the cause, the easier it is to manage the recovery calmly instead of assuming the treatment harmed your teeth.
Immediate Relief at Home What You Can Do Right Now
If your teeth feel sensitive after whitening, the first goal is simple. Lower the triggers and give the teeth a calmer environment for a day or two.
Start with your toothpaste. Desensitizing toothpastes with potassium nitrate are clinically proven to work by blocking pain signals in the tooth’s nerves, and 70% to 85% of patients report significant relief within 48 hours of use, especially when they start before whitening (GoodRx).
Reach for the right ingredients
Look for a toothpaste labeled for sensitive teeth that contains potassium nitrate or stannous fluoride.
- Potassium nitrate: Helps calm the nerve response inside the tooth.
- Stannous fluoride: Helps protect the tooth surface and reduce sensitivity triggers.
Use it consistently. Brush gently twice a day rather than brushing harder in hopes of “cleaning away” the problem.
Change the next few meals
Temperature matters right away. So does acidity.
Choose foods and drinks that are lukewarm or room temperature. Water, scrambled eggs, oatmeal, yogurt if it feels comfortable, pasta, rice, soup that is not hot, and soft foods are usually easier on sensitive teeth than ice water, hot coffee, citrus, or crunchy snacks.
A few easy adjustments help:
- Drink plain water often: Whitening can leave teeth temporarily dehydrated.
- Use a straw when it makes sense: It can reduce direct contact on the front teeth with some beverages.
- Skip acidic foods for now: Citrus, soda, vinegar-heavy dressings, and similar foods can make tenderness feel sharper.
Brush gently, not aggressively
Many people do the wrong thing when teeth feel rough or strange after whitening. They brush harder.
That usually backfires. Use a soft-bristled toothbrush and light pressure. Small circular motions are kinder to enamel and gums than forceful scrubbing.
Tip: If your toothpaste feels too intense because of mint or foaming ingredients, use a small amount and focus on gentle contact rather than a long, aggressive brushing session.
Fluoride can help settle things down
Fluoride rinses or dentist-recommended fluoride products can support recovery by helping the tooth surface remineralize. If you already have one at home, use it as directed. If you have a history of sensitive teeth, ask your dentist which fluoride option fits your situation best.
What usually does not help
Some common reactions make sensitivity worse, not better.
| Better choice | Usually a poor choice |
|---|---|
| Sensitive toothpaste | Whitening toothpaste right after treatment |
| Soft brush | Firm brush or heavy pressure |
| Lukewarm food and drinks | Ice water or very hot coffee |
| A short break between whitening sessions | Repeating whitening too soon |
A short video explanation can also help if you are more visual about home care and recovery:
If you have not whitened yet
The best “home remedy” sometimes starts before treatment. If your teeth have a history of reacting to cold, start a desensitizing toothpaste ahead of time rather than waiting until discomfort begins. Prevention is usually easier than trying to calm an irritated tooth afterward.
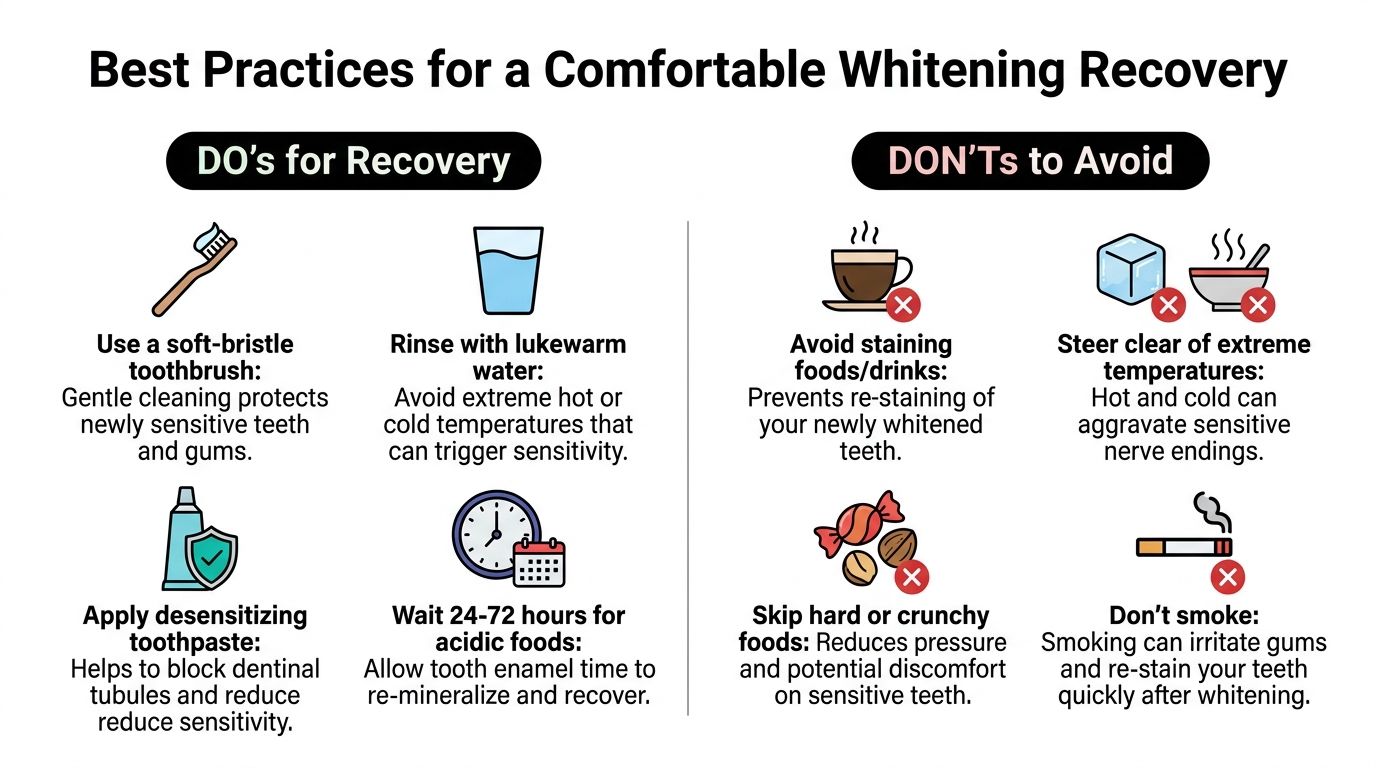
Best Practices for a Comfortable Whitening Recovery
The first stretch after whitening is less about doing more and more about avoiding the mistakes that keep sensitivity active. Small decisions over the next day or two matter.
Clinical guidance notes that post-whitening sensitivity affects up to 78% of patients, and starting a desensitizing toothpaste two weeks before whitening plus avoiding acidic, hot, or cold foods for 24 to 48 hours afterward are effective prevention steps (Andresen DDS).
Do this instead of that
Do
- Use a soft brush: Gentle cleaning keeps plaque under control without irritating the tooth surface or gumline.
- Stick with lukewarm water: That gives reactive teeth fewer reasons to flare up.
- Continue sensitive toothpaste: Recovery goes more smoothly when you stay consistent instead of stopping after one use.
- Give enamel a quiet window: For a short period, choose mild foods and avoid obvious triggers.
Do not
- Do not chase faster whitening: Repeating strips, gels, or touch-ups too soon often causes more discomfort than benefit.
- Do not use abrasive whitening toothpaste: Your teeth do not need extra scrubbing right after bleaching.
- Do not test your teeth with extremes: Sipping ice water “to see if it still hurts” is rarely helpful.
- Do not ignore your baseline sensitivity: If your teeth were already reactive before whitening, recovery may need a slower approach.
A practical recovery rhythm
Many patients do best with a simple routine.
In the morning, brush gently with sensitive toothpaste. Through the day, drink water and keep foods mild. At night, brush gently again and avoid snacking on acidic or very cold foods before bed.
If you want extra guidance on preserving your result while your teeth settle, this article on Teeth Whitening Aftercare offers helpful maintenance tips.
Recovery is part of keeping the result
Comfort and whitening longevity are connected. Teeth that are less irritated are easier to care for well. They are also less likely to push you into inconsistent brushing or rushed touch-ups.
If you want to protect the shade you achieved once sensitivity fades, this guide on how to maintain the results of teeth whitening covers the habits that keep a bright smile looking clean.
Key takeaway: Good whitening aftercare is not only about avoiding pain. It also protects the result you worked for.
How Your Walnut Creek Dentist Prevents Sensitivity From the Start
The biggest difference between professional whitening and a generic kit is not only the gel. It is the planning.
A careful dentist looks at the condition of the enamel, any recession near the gums, existing fillings or crowns, your history of sensitivity, and whether there are untreated issues that should be handled first. Whitening works best when the teeth are healthy enough for it.
Why customization matters
One-size-fits-all trays and strips can leave some areas overloaded and others barely treated. If gel leaks onto the gums or sits unevenly, you may end up with more irritation and less predictable results.
Professional custom trays solve several problems at once. They fit the teeth more precisely, help keep gel where it belongs, and make it easier to use a controlled amount of product. That matters for comfort.
In a randomized controlled trial, a lower concentration of carbamide peroxide caused less tooth sensitivity one day after treatment compared with stronger options, while still producing equivalent color improvement. For many patients, slower and steadier is the smarter path.
The professional trade-offs patients should know
There is always a balance in whitening:
- Stronger and faster: May appeal to patients who want immediate change, but comfort can suffer.
- Lower concentration and longer course: Usually more comfortable and easier for sensitive teeth to tolerate.
- Unsupervised overuse: Tempting when results feel slow, but often the reason sensitivity drags on.
A professional approach also means knowing when not to whiten yet. If someone needs a cleaning and exam first, has gum irritation, or may have cavities or exposed root surfaces, those issues should be addressed before cosmetic treatment starts.
Whitening fits into bigger smile planning
Whitening is often only one part of cosmetic dentistry. Some patients are planning Invisalign. Others are refreshing their smile before crowns or other restorative work. Timing matters because whitening should be coordinated with those decisions, not done in isolation.
That broader view is one reason many people searching for a dentist near me, cosmetic dentist near me, or even general dental care do better with a long-term dental home than with a quick retail whitening option. Good cosmetic treatment is not just about making teeth look lighter. It is about helping them stay healthy and comfortable while you get there.
When Sensitivity Lingers When to Call Dr. Schneider
Most post-whitening sensitivity settles down with home care, time, and a gentler routine. But there is a point where waiting stops being helpful.
Guidance from Derry Family Dentistry notes that if sensitivity persists beyond 48 hours or includes sharp pains, it is time to seek professional intervention, and that a professional-grade fluoride varnish can provide relief for up to 8 weeks (Derry Family Dentistry).
Signs it is time to call
Some symptoms fall outside the normal recovery window.
- Pain that stays strong beyond 48 hours: Especially if it is not improving.
- Sharp, stabbing sensitivity: This can suggest the nerve is more irritated than expected.
- Pain focused in one tooth: That raises the possibility of a crack, cavity, or another issue that whitening happened to uncover.
- Sensitivity that interferes with eating or sleeping: At that point, comfort support should be more active.
What a dentist may check
A good evaluation is not only about confirming that whitening caused the sensitivity. It is about ruling out something else.
Your dentist may look for exposed dentin, gum recession, enamel wear, an old filling with an open margin, a cavity, or signs that the tooth nerve is more inflamed than usual. Sometimes whitening does not create the underlying problem. It makes an existing issue impossible to ignore.
What professional treatment can do
In-office care can go beyond home toothpaste and watchful waiting.
A fluoride varnish may calm the tooth surface more effectively than over-the-counter products. A dentist may also recommend pausing whitening, adjusting future gel strength, shortening tray time, or changing the overall cosmetic plan. If the pain points to another condition, the right treatment could be restorative rather than cosmetic.
Important: Persistent sensitivity is not a sign to push through more whitening. It is a reason to stop and get the tooth checked.
Trust your symptoms
If you are unsure whether your pain counts as “normal,” use a simple standard. If the discomfort is improving, that is reassuring. If it is unchanged, getting worse, or becoming more localized and sharp, it deserves professional attention.
This matters for families and professionals alike in Walnut Creek. A cosmetic concern should never turn into a larger dental problem because someone felt they had to wait it out. The same office that helps with whitening should also be able to guide you if the situation starts to feel more like an emergency dentist question than a routine recovery question.
If you are dealing with sensitivity after whitening or want a more comfortable plan before you begin, William M. Schneider, DDS offers patient-focused dental care for Walnut Creek and the East Bay. From new patient exams and cleanings to cosmetic dentistry, restorative dentistry, and help with urgent dental concerns, the practice is built around clear guidance and comfortable treatment. To talk through your symptoms or schedule a consultation, contact the office at 1855 San Miguel Dr., Suite 31, and take the next step toward a brighter, healthier smile.